It is early on a Monday evening and a young woman is hurried into the maternity ward at Rumginae Hospital in Western Province.
Her pulse is racing, her blood pressure is low, and she lost a lot of blood. She is in shock and needs blood urgently. Without a blood bank, the team must keep Gosima alive while finding a donor and preparing a transfusion.
A new device helps buy that time.
Earlier that day, staff of Rumginae had received an anti-shock garment from UNFPA and the National Department of Health. During the hours preceding Gosima’s arrival, staff had learned how to identify symptoms of haemorrhagic shock during delivery and how to apply the life-saving garment. It was the very garment received that day that Dr Kevin Pondikou wrapped around Gosima that evening.
“We applied the anti-shock garment straight away to help keep her alive while we looked for blood,” shares Dr Kevin the next morning. “By the time the garment was removed, her blood pressure was well controlled. So, the garment was very helpful, and I saw that it worked.”
Gosima received a blood transfusion and both she and her newborn daughter are joined by her mother and sister.
“I’m very happy. It was very easy to apply and easy to remove as well,” said Dr Kevin.
Staff work with Gosima’s sister to piece together what happened to Gosima before arriving at Rumginae. Gosima is 22 years old, and three weeks ago delivered her second child in her village without a midwife or trained birth attendant. Losing blood, she and her mother walked for close to one day to reach Mougolou.
Here, visiting health workers noticed the young woman’s condition and brought her to Kiunga and then to Rumginae. Rumginae Hospital, the closest advanced care facility for women who suffer complications during birth, takes days to reach by road. Patients like Gosima rely on air transport to reach the hospital in emergencies.
For the 14 participants in UNFPA and NDoH’s week-long training, this is the first of many instances in which their new knowledge and skills will help to save women’s lives in North Fly District, Western Province.
Most of these health workers are stationed at centres like Mougolou, with less equipment and fewer staff than Rumginae. Some centres do not have a fridge to safely store oxytocin, the first treatment administered for post-partum haemorrhage. Some have an inconsistent power supply. Many have limited capacity to transport patients to advanced care facilities.
However, for patients like Gosima, these centres are their first point of care in remote communities and their first chance at life-saving interventions. Encouraging women to visit these centres early and training centre staff to know when to refer patients to advanced care facilities and arrange transport is critical.
According to UNFPA's Dr Titilola Duro-Aina, the garment stabilises patients during the delays commonly experienced while evaluating the cause of bleeding or transporting the patient for advanced care.
As Dr Kevin noted when retelling Gosima’s story to other training participants, “The garment kept her alive, while we were identifying and treating the underlying cause which was anaemia”. Advanced care facilities are typically the only place where patients can be treated for such underlying conditions.
The training team consists of experts from UNFPA and the Department of Health who have extensive experience in obstetric care in Papua New Guinea. They make no assumptions about the technical capacities of remote health centres and offer alternatives and solutions that the participants can use in their own facilities. Participants are instructed in how to respond to post-partum hemorrhage, pre-eclampsia and shock, joining simulations and practical activities to build essential skills.
Patient-centred treatment is paramount as the trainers reinforce the need for respectful maternity care. Each facility represented at the training will receive the anti-shock garment to take back to their maternity ward. This piece of equipment, and knowledge of how to use it properly, is a significant boost to the capacity of remote health care providers.
The day after her arrival, Gosima appears far better than when she arrived though remains in a critical condition, needing blood and oxygen. By Wednesday, she has been moved out of the maternity ward in a more stable condition.
Debbie Kupesan from UNFPA gives her a dignity kit which includes reusable pads, slippers and even a torch. These simple kits are a welcome comfort to new mothers and, with the help of UNFPA, are now given to every woman who delivers at Rumginae.
Another woman, Nicrosi Grem, is given a dignity kit from Debbie the same day. She is from Matkomnae, just a short distance from Rumginae, and is joined by family and friends who have come to visit her and her baby.
As Gosima remains under observation with her new daughter, another expectant mother is walking the maternity ward. Pregnant with twins, this woman is staying at Rumginae as a precaution as she is at a higher risk of premature labour. Identifying such risk factors and seeking support early is critical to life-saving maternal health care.
This is why training health workers is just one part of the work UNFPA and NDoH are doing in North Fly. The team is working to encourage women in remote communities to seek out help early by training village health volunteers to educate their communities on how and when women should access community health services. Their hope is that women like Gosima do not have to deliver without skilled support and that no woman has to wait three weeks for emergency medical care.
This project, implemented by UNFPA and the National Department of Health, is funded through the UN Secretary General’s Multi-Partner Trust Fund for COVID-19. The fund seeks to provide support for communities that are vulnerable to COVID-19.
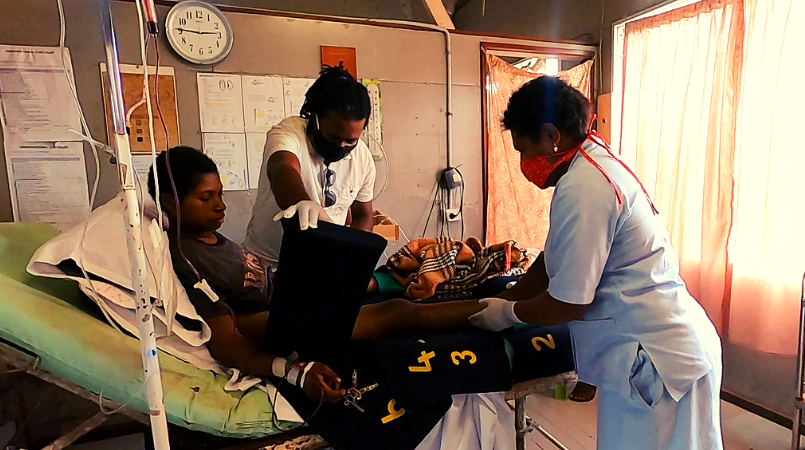
(Dr Kevin Pondikou applies anti-shock garment to Gosima in Rumginae Hospital, Western Province. Photo: UNFPA/ Rachel Donovan)
